HighVolumeHDF

HighVolumeHDF is Fresenius Medical Care
- Reduced mortality risk
- Optimized use of resources with the CorDiax product line
- Lower overall treatment costs
Benefits
Therapy advantages
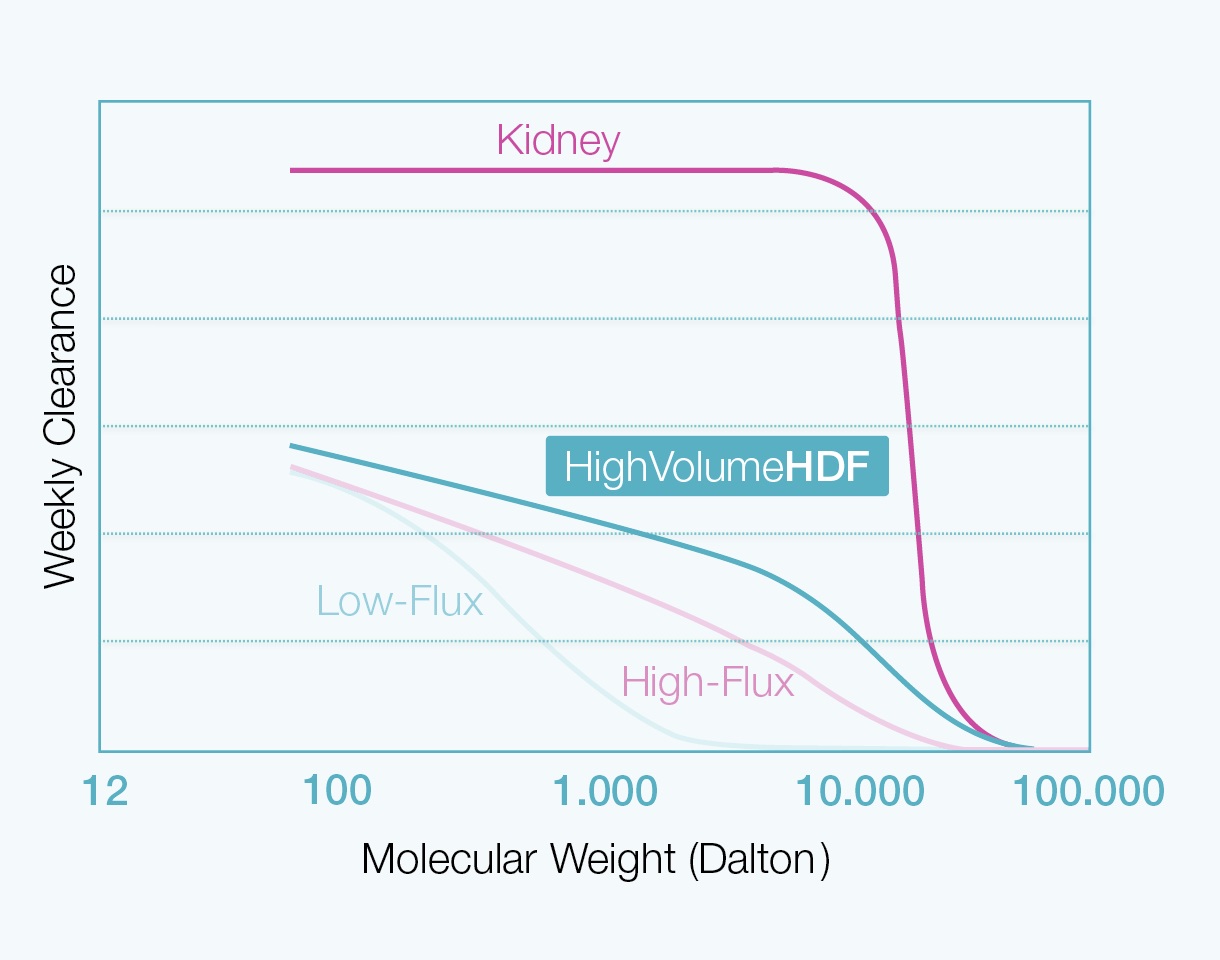
HighVolumeHDF with its numerous positive effects on cardiovascular risk factors in dialysis patients is acknowledged as the most effective dialysis treatment modality1, coming closer to the elimination profile of the natural kidney.
By achieving high substitution volumes, HighVolumeHDF therapy is credited with more effective elimination of middle molecules. HighVolumeHDF improves patient outcomes and exerts beneficial effects on the potential cardiovascular risk factors related to dialysis patients:
- Serum ß2-m and phosphate level2, 3, 4
- Inflammatory response5
- Intradialytic haemodynamic stability6
- Anaemia control9
These factors possibly contribute to improved patient survival.8
Reduced mortality risk with HighVolumeHDF
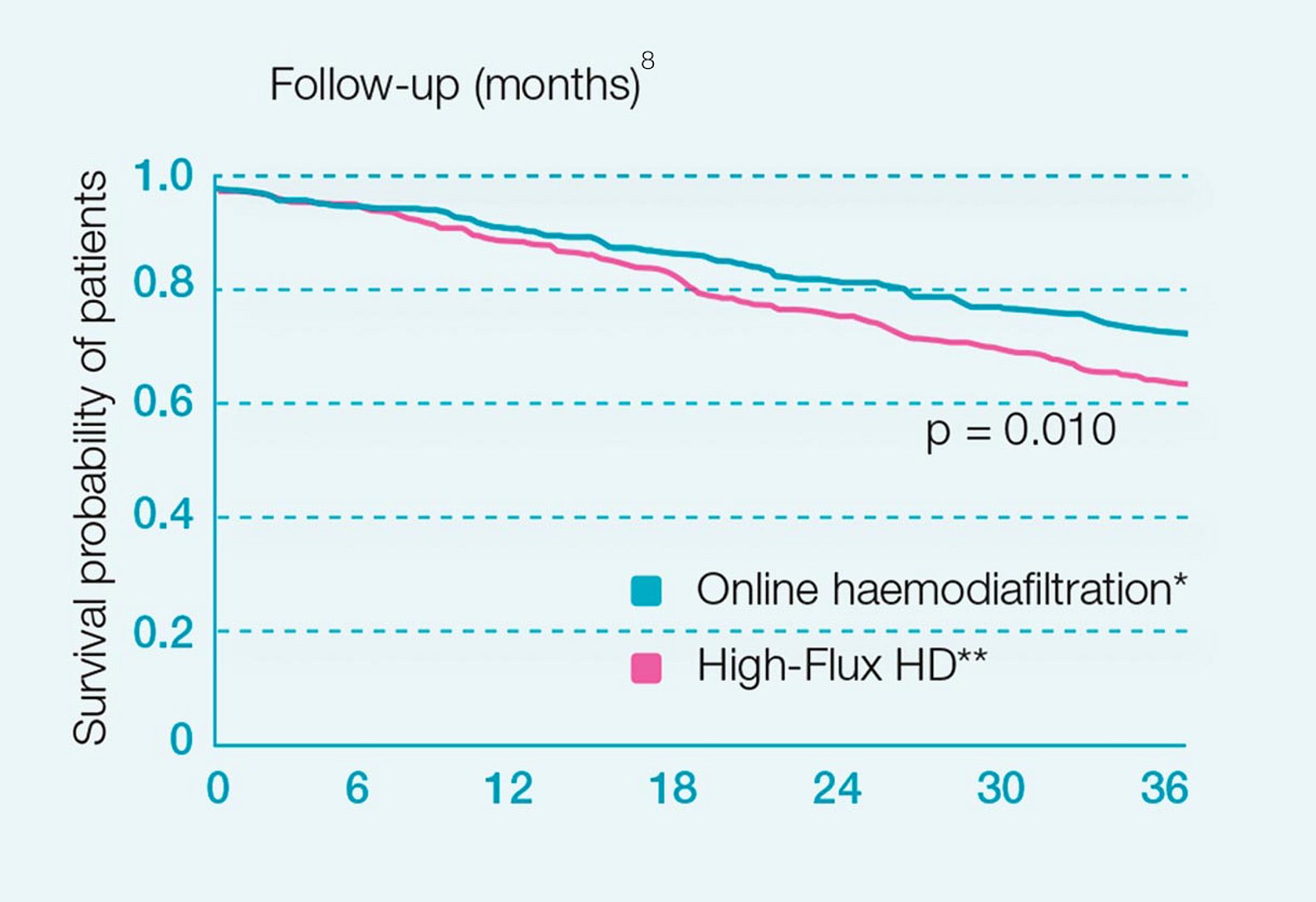
In recent years several studies have confirmed the clinical benefits of HDF8,9,11,12. These studies have demonstrated that large convection volumes in post-dilution mode are required in order to achieve and maximize the benefits of HDF therapy. The Catalonian high-volume HDF study shows a significant 30% risk reduction in all-cause mortality for patients with high-efficiency postdilution online HDF compared to HD8.
The inverse relation between the magnitude of convection volume and mortality risk has been reinforced by the European Dialysis Working Group in their latest meta-analysis13 and was confirmed by the HDF Pooling Project investigators14. The analysis showed that HDF reduces the risk of all-cause and cardiovascular mortality, especially with convection volumes of at least 23 L/session.14
HighVolumeHDF — most advanced and still cost-efficient
It is not only the possible reduction of overall treatment cost which makes HighVolumeHDF with the 5008 CorDiax attractive, but it is also its eco-friendliness and the associated financial savings due to an effective and sustainable use of resources.
Optimized use of resources with the CorDiax product line
The innovative and highly automated features of the CorDiax product line support nursing staff by optimizing daily workflows and ensuring high and consistent levels of patient safety. The result is an easy integration of HighVolumeHDF in the daily routine. The preparation of sterile, non-pyrogenic substitution fluid for HighVolumeHDF is based on a double-stage filtration process.
- No extra costs for an additional single-use filter
- No need for ready-made rinse solutions or waste bag for priming or reinfusion
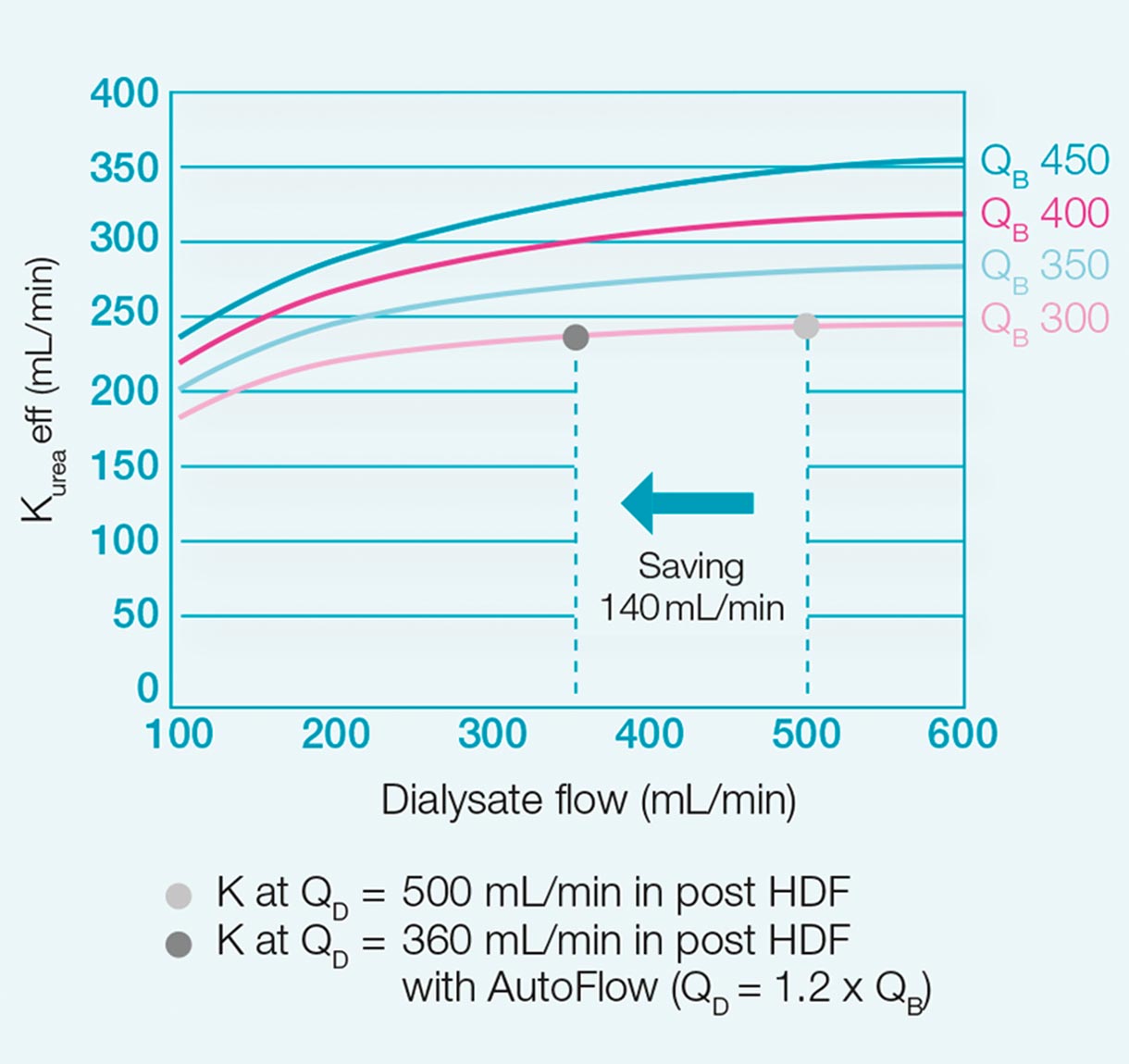
The AutoFlow feature automatically adapts the dialysate flow to the blood flow. This generates substantial savings in water, waste water, concentrates and energy, and results in considerable cost reductions.
HighVolumeHDF — lower overall treatment costs
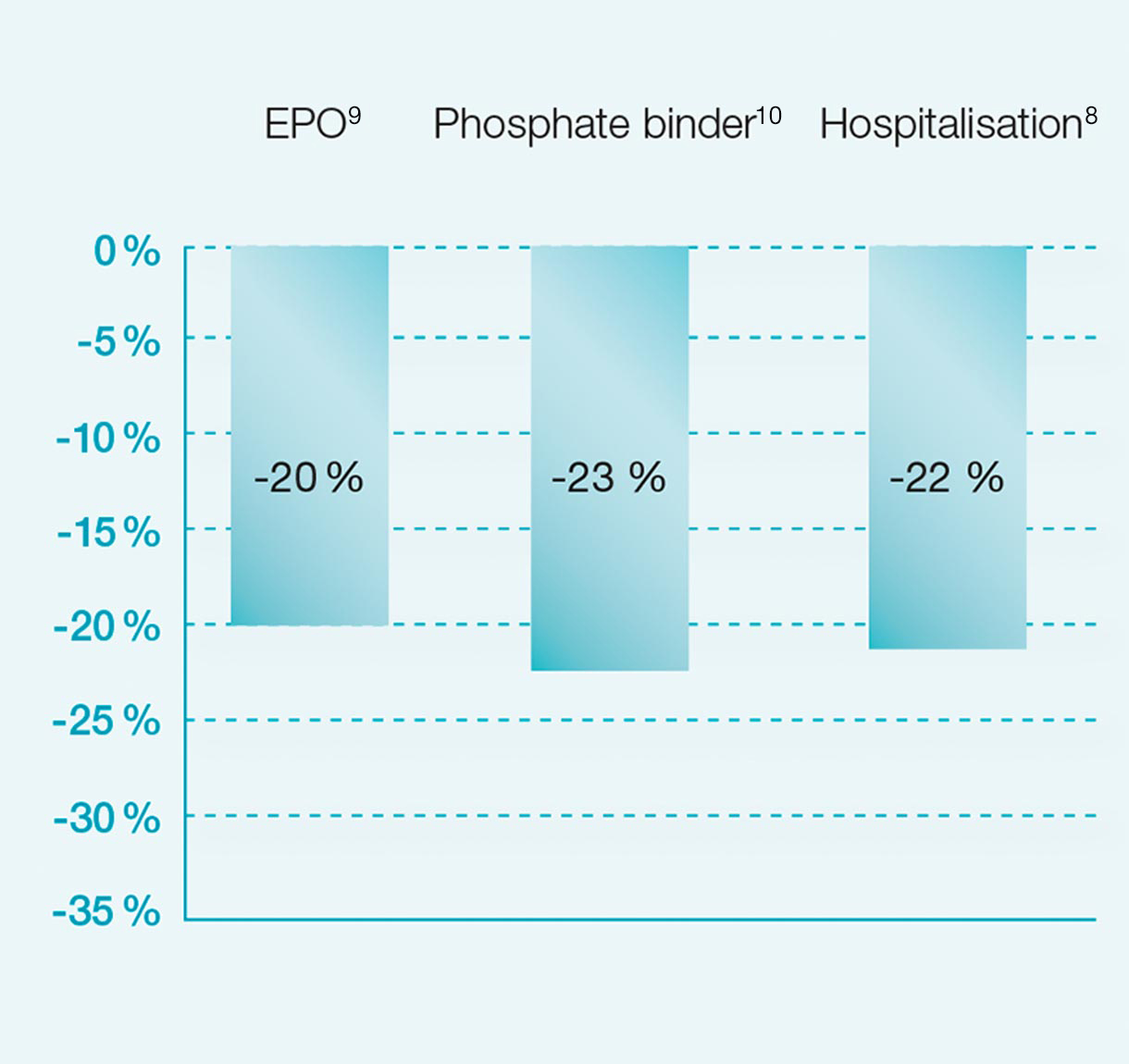
The main drivers for dialysis-related treatment costs are, in addition to direct procedure costs, hospitalization, and erythropoietin (EPO) and phosphate binder usage. In an economically-tight environment every opportunity to reduce the overall treatment cost should be examined. A high hospitalization rate does not only impacting the patients' quality of life but is the most expensive form of medical care in every healthcare system. HighVolumeHDF has the potential to significantly reduce hospitalization rates and hypotensive episodes.8
The amount of EPO1 and phosphate binders4,10 administered to dialysis patients has been shown to be reduced with the application of HDF. Thus, higher quality of care can be provided at a lower medication burden and medication cost.
From promise to proof
Our commitment to achieve the best possible results for every dialysis patient has fuelled our passion for hemodiafiltration (HDF). This passion rests on the firm belief that HDF is the best therapy for every patient.
Our conviction in HDF is now widely shared across the scientific community and backed by evidence. In recent years several publications have already confirmed the benefits of HDF.8,9,11-15. The Catalonian high-volume HDF study8 provides accumulating evidence for the benefits of this therapy. Convincing scientific evidence for significantly improved patient outcomes combined with the simple and reliable use of the 5008 CorDiax are compelling reasons to switch to HighVolumeHDF – now.
That’s why for more than 30 years Fresenius Medical Care has been developing products for Cardioprotective Hemodialysis, leading to the CorDiax product line — which perfectly supports the application of HighVolumeHDF therapy.
From hemodiafiltration to HighVolumeHDF
HDF is a renal replacement technique combining two principles – diffusion and convection. The convective process is based on the ultrafiltration of large amounts of plasma water across the membrane. This allows for the effective removal of larger solutes due to convection in addition to the diffusive transport of small molecules.
To maintain the fluid balance it is necessary to replace the additional ultrafiltration volume, ideally after the dialyzer, the so-called post-dilution HDF.
Volume matters in hemodiafiltration
Recent publications have demonstrated that a large convective volume in post-dilution mode is required in order to maximize the benefits of HDF therapy.8, 9,11-15
According to the Catalonian high-volume HDF study a substitution volume (without allowing for weight loss) of at least 21 L per treatment in post-dilution mode should be the target to derive the survival benefit.8
The production of large amounts of substitution volume is no longer a challenge. Today maximizing substitution volume for each patient requires a new therapeutic approach — HighVolumeHDF.
Study
The Catalonian high-volume HDF study8
The Catalonian high-volume HDF study data confirm our original conviction that every patient should get the chance to benefit from HighVolumeHDF.
Improved Survival
| 30% | risk reduction in all-cause mortality (p=0.01) |
|---|---|
| 55% | risk reduction in mortality from infection (p=0.03) |
| 61% | risk reduction in mortality from stroke (p=0.03) |
Compared with patients maintained on conventional high-flux hemodialysis, those randomized to high-efficiency postdilution online hemodiafiltration had significantly lower all-cause mortality.
Better patients‘ well-being
| 28% | risk reduction in incidence of hypotensive episodes (p<0.001) |
|---|
Reduced treatment costs
| 22% | risk reduction in all-cause hospitalization (p=0.001) |
|---|
Study details8
Study aim:
To compare the impact of online hemodiafiltration over hemodialysis on patient survival.
Study design:
Multi-center, prospective randomized controlled trial promoted by the Catalonian Society of Nephrology.
Study endpoints:
The primary outcome variable was all-cause mortality, and secondary outcomes included cardiovascular mortality, all-cause hospitalization, treatment tolerance and laboratory data.
Patients:
906 chronic hemodialysis patients were assigned either to continue hemodialysis (n=450) or to be switched to high-efficiency postdilution online hemodiafiltration (n=456).
Products

HighVolumeHDF is Fresenius Medical Care
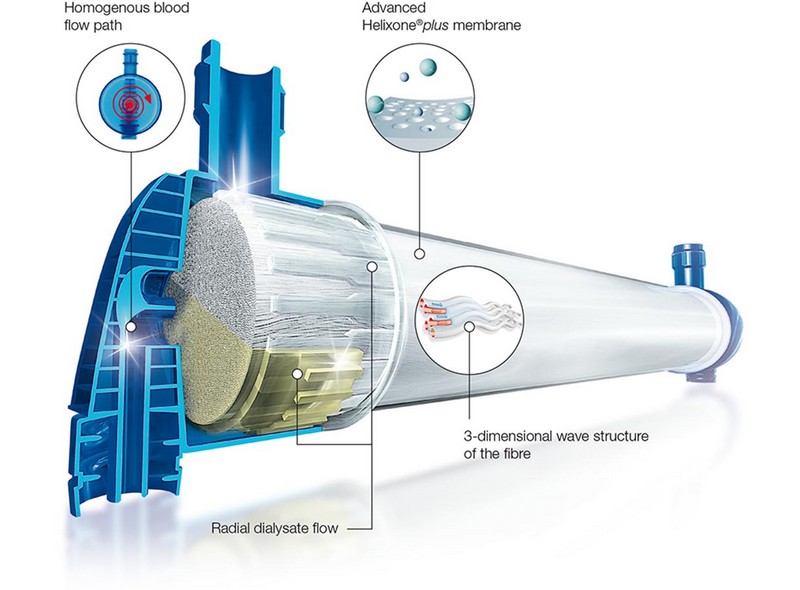
The challenges of hemodiafiltration have led us to continuously develop new innovative products, which support the HighVolumeHDF therapy approach. Our long standing commitment to making HighVolumeHDF available to all patients has resulted in an advanced and highly synergetic portfolio. The result: The 5008 CorDiax and 5008S CorDiax in combination with the FX CorDiax HDF hemodiafilter and the Online Purification Cascade (OPC) today form an integrated therapy system, enhanced by services tailored to support your therapy.

5008 CorDiax and 5008S CorDiax: HighVolumeHDF as standard
With the new AutoSubplus function of the 5008 CorDiax and the 5008S CorDiax, HighVolumeHDF has become as simple and reliable as HD without any need for additional user interaction.

Online Purification Cascade (OPC): Intelligent water quality management
The OPC product line covers all processes for the delivery of the large amounts of substitution fluids required for HighVolumeHDF therapy.
Learn more about Water technology
1 Krick G, Ronco C (eds), Contributions to Nephrology (2011); 175: 93-109.
2 Canaud B., Contributions to Nephrology (2007); 158: 216-224.
3 Penne L. et al., Clinical Journal of the American Society of Nephrology (2010); 5: 80-86.
4 Davenport A., Nephrology Dialysis Transplantation (2010); 25: 897-901.
5 Pedrini L. et al., Nephrology Dialysis Transplantation (2011); 26: 2617-2624.
6 Locatelli F. et al., Journal of the American Society of Nephrology (2010); 21: 1798-1807.
7 Bonforte G. et al., Blood Purification (2002); 20: 357-363.
8 Maduell F. et al., Journal of the American Society of Nephrology (2013); 24: 487-497.
9 Ok E., et al., Nephrology Dialysis Transplantation (2013); 28: 192-202.
10 Pedrini, L. et al., Nephrology Dialysis Transplantation (2011); 26: 2617-2624.
11 Grooteman M.P. et al., Journal of the American Society of Nephrology (2012); 23(6): 1087-96.
12 Canaud B. et al., Kidney International (2006); 69(11): 2087-93.
13 Mostovaya I.M. et al., Seminars in Dialysis (2014); 27(2): 119-127.
14 Peters S.A.E. et al., Nephrology Dialysis Transplantation (2016); 31: 978-984.
15 Basile C. et al., Journal of Nephrology (2017); 30(2): 181-186.